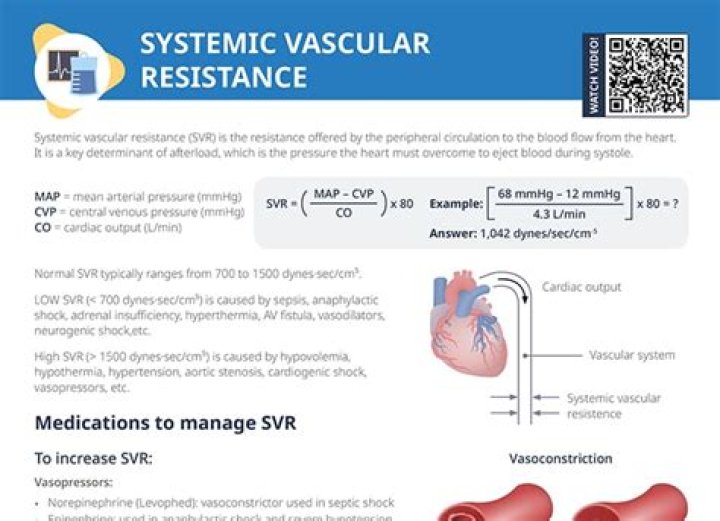
Vascular resistance. The resistance offered by the systemic circulation is known as the systemic vascular resistance (SVR) or may sometimes be called by the older term total peripheral resistance (TPR), while the resistance offered by the pulmonary circulation is known as the pulmonary vascular resistance (PVR)..
Similarly, is peripheral vascular resistance the same as systemic vascular resistance?
Systemic Vascular Resistance. Systemic vascular resistance (SVR) is sometimes known as total peripheral resistance (TPR) or peripheral vascular resistance (PVR). But don't get this PVR confused with another PVR, pulmonary vascular resistance! They're totally not the same thing.
Similarly, what is the difference between afterload and systemic vascular resistance? Afterload is the pressure the myocardial muscle must overcome to push blood out of the heart during systole. The left ventricle ejects blood through the aortic valve against the high pressure of the systemic circulation, also known as systemic vascular resistance (SVR).
Likewise, what is peripheral vascular resistance?
Peripheral resistance is the resistance of the arteries to blood flow. As the arteries constrict, the resistance increases and as they dilate, resistance decreases. Peripheral resistance is determined by three factors: Autonomic activity: sympathetic activity constricts peripheral arteries.
What causes peripheral vascular resistance?
Vascular resistance is used to maintain organ perfusion. In certain disease states, such as congestive heart failure, there is a hyper-adrenergic response, causing an increase in peripheral vascular resistance. Prolonged increases in blood pressure affect several organs throughout the body.
Related Question Answers
What is the most important determinant of vascular resistance?
The major determinant of vascular resistance is small arteriolar (known as resistance arterioles) tone. These vessels are from 450 µm down to 100 µm in diameter. (As a comparison, the diameter of a capillary is about 5 to 10 µm.) Another determinant of vascular resistance is the pre-capillary arterioles.How does peripheral vascular resistance affect blood pressure?
Increases in peripheral resistance, blood volume, and cardiac output result in higher blood pressure. Conversely decreases in any of these factors lead to lower blood pressure. Three main sources of peripheral resistance: Blood vessel diameter, blood viscosity, and total vessel length.What does systemic vascular resistance measure?
Systemic vascular resistance is defined as the systemic mean arterial blood pressure minus right arterial pressure divided by cardiac output.What is meant by systemic vascular resistance?
Systemic vascular resistance (SVR) refers to the resistance to blood flow offered by all of the systemic vasculature, excluding the pulmonary vasculature. This is sometimes referred as total peripheral resistance (TPR).How can systemic vascular resistance be reduced?
Reduce Systemic Vascular Resistance An effective and inexpensive way of reducing venous pressure and cardiac output is by using drugs that reduce blood volume. These drugs (diuretics) act on the kidney to enhance sodium and water excretion.What happens when total peripheral resistance increases?
Total peripheral resistance We increased the pressure by decreasing the space the flow of water could go through. The same principle applies in the body with blood and the vessels. In cardiovascular terms this is known as 'total peripheral resistance' (TPR).Why does systemic vascular resistance decrease with exercise?
BACKGROUND: Systemic vascular resistance falls in exercise as a consequence of metabolically-linked vasodilatation in active skeletal muscles. Recovery of normal resting skeletal muscle tissue oxygen tension and skeletal muscle vascular tone after exercise depends on the post-exercise recovery process.What are the major sites of resistance in the systemic vascular system?
The distribution of blood flow is regulated by changes in vascular resistance. The arterioles are the primary site of variable resistance in the systemic circulation. Arterioles are small in diameter and few in number so their total cross sectional area is the smallest.Why is total peripheral resistance important?
Blood flow decreases when there is increased resistance to its flow. Total peripheral resistance is defined as the total resistance to flow of blood in the systemic circulation. The arterioles are important regulators of blood flow because of their smaller size and muscular walls.What factors affect peripheral circulation?
Four major factors interact to affect blood pressure: cardiac output, blood volume, peripheral resistance, and viscosity.What does total peripheral resistance mean?
Systemic Vascular Resistance. Systemic vascular resistance (SVR) refers to the resistance to blood flow offered by all of the systemic vasculature, excluding the pulmonary vasculature. This is sometimes referred as total peripheral resistance (TPR).How do you measure peripheral resistance?
Total peripheral resistance (TPR) is determined as the quotient of ModelFlow-derived MAP divided by CO. TPRest was obtained as the quotient of mean arterial pressure in millimeters of mercury (mmHg) divided by cardiac output in liters per minute (L/min) [Equation 2].How does vascular resistance affect blood flow?
The slowing or blocking of blood flow is called resistance. In the arterial system, as resistance increases, blood pressure increases and flow decreases. In the venous system, constriction increases blood pressure as it does in arteries; the increasing pressure helps to return blood to the heart.What does increased SVR mean?
Systemic Vascular Resistance (SVR): The measurement of resistance or impediment of the systemic vascular bed to blood flow. An increased SVR can be caused by vasoconstrictors, hypovolemia, or late septic shock. A decreased SVR can be caused by early septic shock, vasodilators, morphine, nitrates, or hypercarbia.What happens to total peripheral resistance during exercise?
The decrease in total peripheral resistance is the result of decreased vascular resistance in skeletal muscle vascu- lar beds, leading to increased blood flow. The increase in blood flow to cardiac and skeletal muscle produced by exercise is called exercise hyperemia.In which blood vessels is blood pressure highest?
Each time the heart beats (contracts and relaxes), pressure is created inside the arteries. The pressure is greatest when blood is pumped out of the heart into the arteries. When the heart relaxes between beats (blood is not moving out of the heart), the pressure falls in the arteries.Why is pulmonary vascular resistance low?
The increase in pulmonary vascular resistance at very low lung volume is caused by the decrease in caliber of the extra-alveolar vessels. Because these vessels are normally held open by the radial traction of the surrounding parenchyma, their caliber is least in the collapsed lung.Why would you want to decrease preload?
Ventricular preload is decreased by: Decreased venous blood pressure, most commonly resulting from reduced blood volume (e.g., hemorrhage) or gravity causing blood to pool in the lower limbs when standing upright. Impaired atrial contraction that can result from atrial arrhythmias such as atrial fibrillation.What affects preload?
Factors affecting preload Preload is affected by venous blood pressure and the rate of venous return. These are affected by venous tone and volume of circulating blood. Preload is related to the ventricular end-diastolic volume; a higher end-diastolic volume implies a higher preload.