What is the color of Staphylococcus epidermidis?
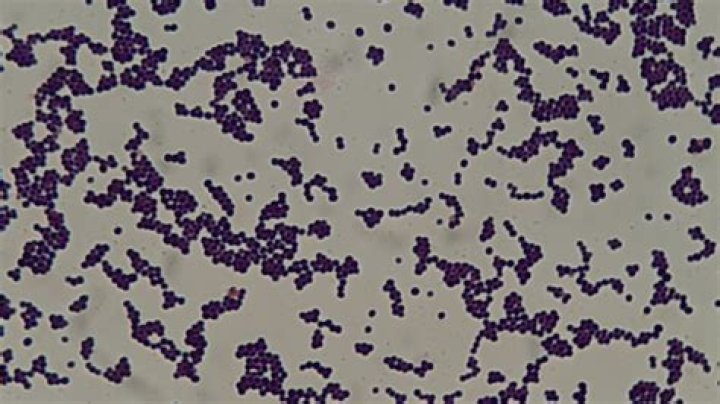
.
Simply so, what infections does Staphylococcus epidermidis cause?
Staph. epidermidis is a common cause of infections involving indwelling foreign devices, surgical wound infections, and bacteremia in immunocompromised patients. The occult nature of these infections and low virulence of the organism make diagnosis and treatment difficult.
Similarly, is Staphylococcus epidermidis good or bad? Staphylococcus epidermidis and other coagulase-negative staphylococci (CoNS), once considered nonpathogenic commensal organisms, now are recognized clearly as potential true pathogens, particularly in hospitalized patients and those with indwelling foreign bodies.
Also asked, how is Staphylococcus aureus different from Staphylococcus epidermidis?
Staphylococcus aureus produce yellow colonies with yellow zones, whereas other Staphylococci produce small pink or red colonies with no colour change to the medium. If an organism can ferment mannitol, an acidic byproduct is formed that will cause the phenol red in the agar to turn yellow.
How is Staphylococcus epidermidis diagnosed?
To diagnose a staph infection, your doctor will:
- Perform a physical exam. During the exam, your doctor will closely examine any skin lesions you may have.
- Collect a sample for testing. Most often, doctors diagnose staph infections by checking a tissue sample or nasal secretions for signs of the bacteria.
What kills Staphylococcus epidermidis?
Methicillin-resistant Staphylococcus aureus (MRSA) is highly resistant to treatment with antibiotics. These include oxacillin, flucloxacillin, and dicloxacillin. Through their research, they were able to show that a type of probiotic bacteria called Bacillus is able to fight and effectively eliminate S. aureus.How do you get Staphylococcus epidermidis?
Staphylococcus epidermidis. Infections are associated with intravascular devices (prosthetic heart valves, shunts, etc.) but also commonly occur in prosthetic joints, catheters, and large wounds. Catheter infections along with catheter-induced UTIs lead to serious inflammation and pus secretion.Where is Staphylococcus epidermidis found on the body?
Staphylococcus epidermidis lives on everyone's skin. The bacteria prefer sweaty places, such as your armpits, but are also found on your back and in your nostrils. Together with other micro-organisms, they produce substances from sweat, bringing about the body odour associated with perspiration.How long is staph contagious?
How long is the contagious period for a staph infection? Most staph skin infections are cured with antibiotics; with antibiotic treatment, many skin infections are no longer contagious after about 24-48 hours of appropriate therapy. Some skin infections, such as those due to MRSA, may require longer treatment.Is Staph epidermidis contagious?
Most staph bacteria are transmitted by person-to-person contact, but viable staph on surfaces of clothing, sinks, and other objects can contact skin and cause infections. As long as a person has an active infection, the organisms are contagious.How can Staphylococcus epidermidis be prevented?
Preventing Staph Infection- Keep your hands clean by washing them thoroughly with soap and water.
- Keep cuts and scrapes clean and covered with bandages until they heal.
- Avoid contact with other people's wounds or bandages.
- Do not share personal items such as towels, clothing, or cosmetics.
What is Staphylococcus epidermidis resistant to?
epidermidis strains are resistant to methicillin (oxacillin) (Farrell et al., 2011). Resistance to multiple antibiotics (such as methicillin and vancomycin) is a major obstacle in the treatment of infections caused by Staphylococcus spp.What are the symptoms of Staphylococcus epidermidis?
What are the symptoms of staph infections?- Skin infections can look like pimples or boils.
- Bone infections can cause pain, swelling, warmth, and redness in the infected area.
- Endocarditis causes some flu-like symptoms: fever, chills, and fatigue.



