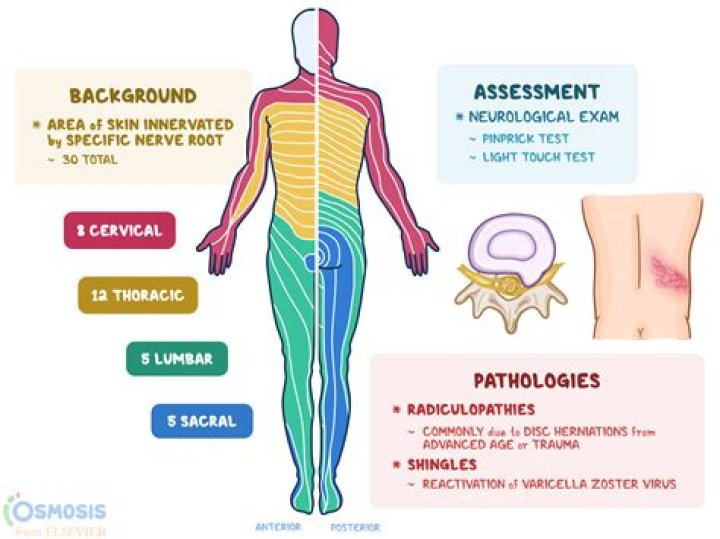
The dermatome pattern for the S1 nerve root that is most commonly described in the literature involves the posterolateral thigh and leg and the lateral foot. It is known that the lower extremity referred pain pattern of somatic structures innervated by the S1 segment also commonly follows the classic S1 dermatome [53]..
Simply so, what does the s1 nerve control?
(Numbness for the S1 nerve runs on the outside of the foot. The S1 nerve root also supplies innervation for the ankle jerk (tap on the achilles tendon and the foot goes down), and a loss of this reflex indicates S1 impingement, although it does not create loss of function.
Likewise, what do Dermatomes tell you? Spinal nerves help to relay information from other parts of your body to your central nervous system. As such, each dermatome transmits sensory details from a particular area of skin back to your brain. Dermatomes can be helpful in evaluating and diagnosing conditions affecting the spine or nerve roots.
Additionally, what is S 1 radiculopathy?
Lumbar radiculopathy Lumbar radiculopathy is a condition in wich pain is caused in the lower back and hip radiating down the back of the thigh into the leg. It is caused by damage to one of the lower segments of the spine, ranging from L1 to S1 caused by compression of the nerve roots which exit the spine.
What are symptoms of s1 nerve damage?
Compression or inflammation of the L5 and/or S1 spinal nerve root may cause radiculopathy symptoms or sciatica, characterized by:
- Pain, generally felt as a sharp, shooting, and/or searing feeling in the buttock, thigh, leg, foot, and/or toes.
- Numbness in the foot and/or toes.
Related Question Answers
How do you treat l5 s1 pain?
Treatment of L5-S1 usually begins with: Medication. Over-the-counter (OTC) medications, such as non-steroidal anti-inflammatory drugs (NSAIDs) are usually tried first for pain stemming from L5-S1. For more severe pain, prescription medication, such as opioids, tramadol, and/or corticosteroids may be used.Can l5 s1 cause hip pain?
The presenting history of gradual hip pain without trauma, as well as numbness and tingling down the leg, leads to a differential diagnosis between hip and low back pathology. The imaging was the linchpin of the diagnosis with no hip pathology revealed, and significant degenerative changes noted at L4-L5 and L5-S1.Can you prove nerve damage?
Objectively Documenting Nerve Damage While the plaintiff can never establish the exact dollar value of the nerve damage pain and suffering, proving objectively that nerve damage occurred is possible. Diagnostic nerve conduction tests can show impairment of nerves.Can l5 s1 cause paralysis?
Conclusion: A syndrome with perianal sensory deficit, paralysis of the sphincter, and sexual dysfunction may occur in patients with lumbar L5-S1 disc disease.What part of the spine is s1?
Sacral region (bottom of the spine) - located below the lumbar spine, the sacrum is a series of 5 bony segments fused together (known as S1 to S5) that create a triangular-shaped bone that serves as the base of the spine and makes up part of the pelvis.The segment where the lumbar spine meets the sacral region, L5-S1,How is l5 s1 disc bulge treated?
How Do I Heal My Moderate Herniated Disc at L5-S1? - Avoid the Common Causes. First of all, before back pain can be resolved, the source of the pain must be identified.
- Bed Rest.
- Non-Steroidal Anti-Inflammatory Drugs.
- Perform Healing Exercises.
- Flex and Extensions.
What is s1 in your back?
The lumbosacral joint, also called L5-S1, is a term used to describe a part of the spine. In fact, L5-S1 is the exact spot where the ?lumbar spine ends and the sacral spine begins. It is composed of the last bone in the low back, called L5, and the triangularly shaped bone beneath, known as the sacrum.Do pinched nerves show up on MRI?
MRI is sensitive to changes in cartilage and bone structure resulting from injury, disease, or aging. It can detect herniated discs, pinched nerves, spinal tumors, spinal cord compression, and fractures.How is s1 radiculopathy treated?
Radiculopathy Treatment Weight loss strategies to reduce pressure on the problem area. Physical therapy to strengthen the muscles and prevent further damage. Steroid injections to reduce inflammation and relieve pain.Is radiculopathy a chronic condition?
Radiculopathy is a condition due to a compressed nerve in the spine that can cause pain, numbness, tingling, or weakness along the course of the nerve. Radiculopathy can occur in any part of the spine, but it is most common in the lower back (lumbar radiculopathy) and in the neck (cervical radiculopathy).Can lumbar radiculopathy cause paralysis?
Lumbar radiculopathy is pressure on one of the nerve roots in your lower back. It can cause hip pain and sciatica, or shooting pain in your leg. Incontinence, sexual dysfunction, or paralysis can also occur in severe cases.How long does it take for lumbar radiculopathy to heal?
What is the treatment for lumbar radiculopathy? Most spine problems heal over time without surgery in 6 to 12 weeks. They often respond to rest and self-care. Avoid activities that increase the pain in the leg such as bending, running, heavy lifting or strenuous activity.What is the difference between sciatica and radiculopathy?
Lumbar Radiculopathy (Nerve Root Compression) Lumbar radiculopathy refers to disease involving the lumbar spinal nerve root. Sciatica is the term often used by laypeople. Lumbar radiculopathy is typically caused by a compression of the spinal nerve root.How do you test for radiculopathy?
The foraminal compression test, or Spurling test, is probably the best test for confirming the diagnosis of cervical radiculopathy. It is performed by positioning the patient with the neck extended and the head rotated, and then applying downward pressure on the head.Is radiculopathy a disability?
Can someone with cervical radiculopathy (pinched nerve) receive Social Security Disability Benefits? Cervical radiculopathy can be caused by trauma, degenerative changes or anything that puts pressure on the nerve root. While you may have neck pain, you may also have symptoms in your hands.What is the best painkiller for nerve pain?
Painkilling medicines. Some people with neuropathic pain turn to familiar over-the-counter painkillers like acetaminophen, aspirin, and ibuprofen. While these drugs might help with mild or occasional pain, they're often not strong enough for serious nerve pain.What does the t12 nerve control?
Thoracic Spinal Nerves. The thoracic spine has 12 nerve roots (T1 to T12) on each side of the spine that branch from the spinal cord and control motor and sensory signals mostly for the upper back, chest, and abdomen. Each thoracic spinal nerve is named for the vertebra above it.What causes Dermatomes?
A dermatome is an area of skin supplied by sensory neurons that arise from a spinal nerve ganglion. Symptoms that follow a dermatome (e.g. like pain or a rash) may indicate a pathology that involves the related nerve root. Examples include somatic dysfunction of the spine or viral infection.Why are there no Dermatomes on the face?
As it relates to skin innervation of the face and neck there is also contribution from the cervical spinal nerves (C2, C3, C4). Note: The spinal nerve at C1 lacks any significant afferent input from the skin and thus is the only spinal nerve without any representation as a dermatome.