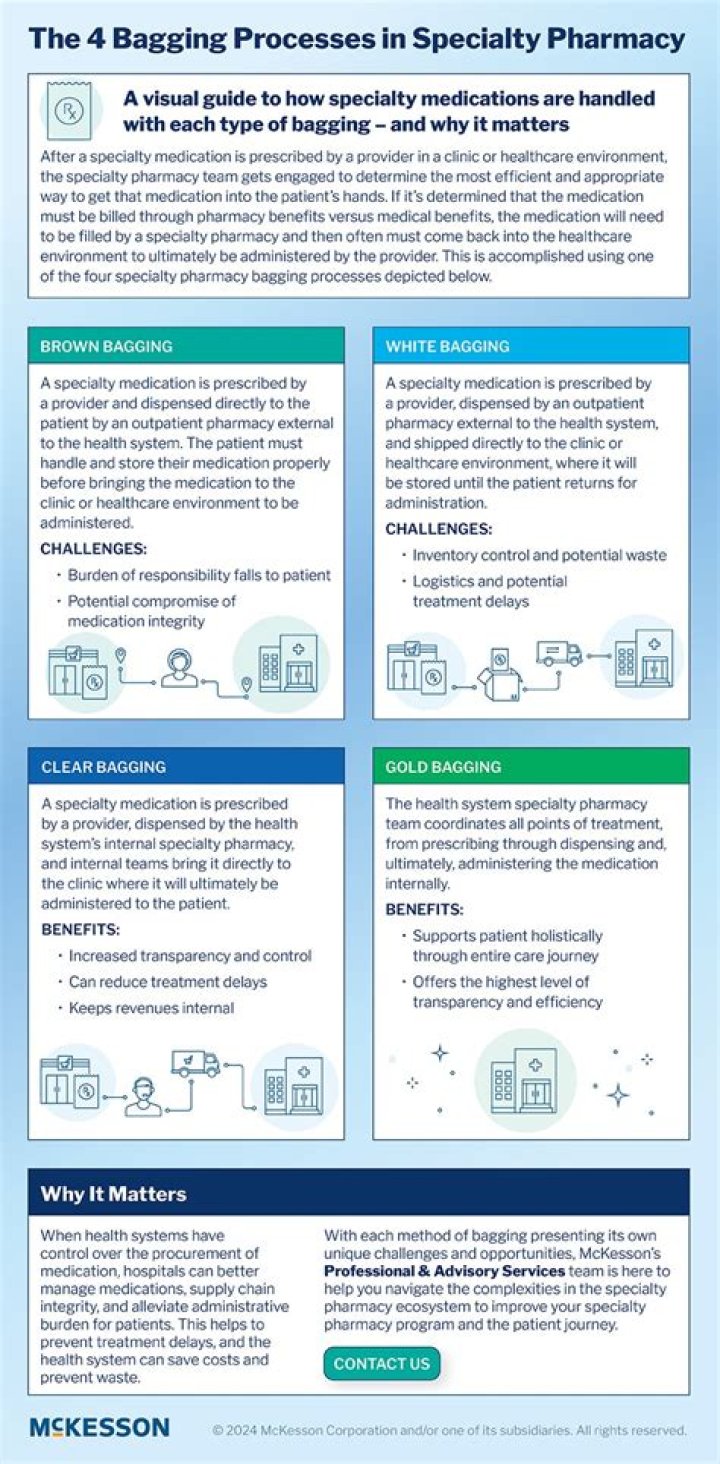
Clear bagging occurs when the health system's specialty pharmacy delivers medication to the clinic. Their thought is that if a medication must be shipped to the infusion center, it must come from their own specialty pharmacy or through buy-and-bill..
Regarding this, what is white bagging in pharmacy?
White bagging is the method of delivery by which physician-administered drugs are dispensed by a specialty pharmacy (SP) for a specific patient, shipped to the physician for administration, and generally paid under the pharmacy benefit rather than the medical benefit.
Subsequently, question is, is the medication buy and Bill? The process is called buy-and-bill, because the medical claim is submitted after the provider has purchased and administered the drug. Thus, in the buy-and-bill system, the provider is responsible for: Ordering and purchasing the drug. Managing drug inventory at the practice.
Subsequently, one may also ask, what is brown bagging in pharmacy?
“Brown bagging” is when a patient acquires specialty medication from a pharmacy and takes it to the physician's office for administration. With white bagging, providers need to stock and store the medication for each patient, keeping it separate from hospital and office stocks, which can be logistically challenging.
What is a buy and Bill?
In the buy-and-bill process, a healthcare provider purchases a drug from a pharmaceutical wholesaler or specialty distributor. After administering the drug, the provider submits a claim for reimbursement for the drug and any other medical services. The provider holds the product until the patient arrives for treatment.
Related Question Answers
How do you bill for medication management?
For the medication management described, the best choice is the standard E/M codes for a new or established patient. In the outpatient setting, the codes are 99201-99215. Question: In my outpatient practice I often see patients for medication management and previously used CPT® code 90862, which was deleted for 2013.What is the difference between medical benefit and pharmacy benefit?
These therapies are managed across different benefit structures for medication reimbursement, including the medical, pharmacy, and separate specialty pharmacy benefits. The only difference from a pharmacy standpoint is how and where to submit the claims.What is a J code?
J codes are a subset of the HCPCS Level II code set used to primarily identify injectable drugs. A J code may cover the supply, injection or infusion of a drug or biological. Drugs dispensed to a patient and immunizations are likely not covered by a J code.What is a hub in specialty pharmacy?
Hub services are a growing market of offerings that allow manufacturers to maintain a connection with patients during all phases of the prescription delivery process. For manufacturers of specialty drugs, the ability to have a single point of contact for their therapies helps ensure efficient medication distribution.What is specialty distribution?
Small specialty pharmacies and retail pharmacies that handle specialty pharmaceuticals use the services of a specialty wholesaler (sometimes called specialty distributors). The largest specialty pharmacies are owned by PBMs or large retailers.What does a specialty pharmacy do?
Specialty pharmacy refers to distribution channels designed to handle specialty drugs — pharmaceutical therapies that are either high cost, high complexity and/or high touch. Patients typically pay the same co-payments whether or not their insurers cover the drug."What type of company is McKesson?
McKesson Corporation is an American company distributing pharmaceuticals and providing health information technology, medical supplies, and care management tools.