What are the signs of hemolytic transfusion reaction?
- Back pain.
- Bloody urine.
- Chills.
- Fainting or dizziness.
- Fever.
- Flank pain.
- Flushing of the skin.
.
Similarly, it is asked, what is the most common symptom of a hemolytic transfusion reaction?
The most common signs and symptoms include fever, chills, urticaria (hives), and itching. Some symptoms resolve with little or no treatment. However, respiratory distress, high fever, hypotension (low blood pressure), and red urine (hemoglobinuria) can indicate a more serious reaction.
One may also ask, what do you do for a hemolytic transfusion reaction? Hemolytic transfusion reactions are treated as follows:
- Stop transfusion as soon as a reaction is suspected.
- Replace the donor blood with normal saline.
- Examine the blood to determine if the patient was the intended recipient and then send the unit back to the blood bank.
Also to know is, what is used to diagnose a hemolytic transfusion reaction?
Diagnosis. The diagnosis of AHTR is made with microscopic examination of the recipient's blood and a direct antiglobulin test. The donor and recipient blood can be re-tested with a type, crossmatch, and antibody screen to determine the cause of the reaction.
What are the signs and symptoms of a hemolytic reaction?
Transfusion reaction symptoms include:
- back pain.
- dark urine.
- chills.
- fainting or dizziness.
- fever.
- flank pain.
- skin flushing.
- shortness of breath.
What is the most dangerous type of blood transfusion reaction?
The most common immediate adverse reactions to transfusion are fever, chills and urticaria. The most potentially significant reactions include acute and delayed haemolytic transfusion reactions and bacterial contamination of blood products.What is the most common transfusion reaction?
Febrile non-hemolytic transfusion reactions are the most common reaction reported after a transfusion. FNHTR is characterized by fever or chills in the absence of hemolysis (breakdown of red blood cells) occurring in the patient during or up to 4 hours after a transfusion.What happens if someone receives the wrong blood type?
Transfusion with the wrong blood type can cause a severe reaction that may be life-threatening. If you have many blood transfusions, you are more likely to have problems from immune system reactions. A reaction causes your body to form antibodies that attack the new blood cells. But tests can help avoid this.What does hemolytic reaction mean?
A hemolytic transfusion reaction is a serious complication that can occur after a blood transfusion. The reaction occurs when the red blood cells that were given during the transfusion are destroyed by the person's immune system. There are other types of allergic transfusion reactions that do not cause hemolysis.What are the different types of transfusion reactions their causes and symptoms?
Acute transfusion reactions are typically classified into the following entities :- Transfusion-related acute lung injury (TRALI)
- Circulatory (volume) overload.
- Bacterial contamination and endotoxemia.
- Acute hemolytic reactions.
- Nonhemolytic febrile reactions.
- Allergic reactions.
How long after a blood transfusion can a reaction occur?
DELAYED HEMOLYTIC REACTION Not all hemolytic reactions occur during or shortly after blood transfusion. The so-called “delayed” hemolytic reaction commonly occurs 4 - 8 days after blood transfusion, but may develop up to 2 weeks later.How many transfusions can a person have?
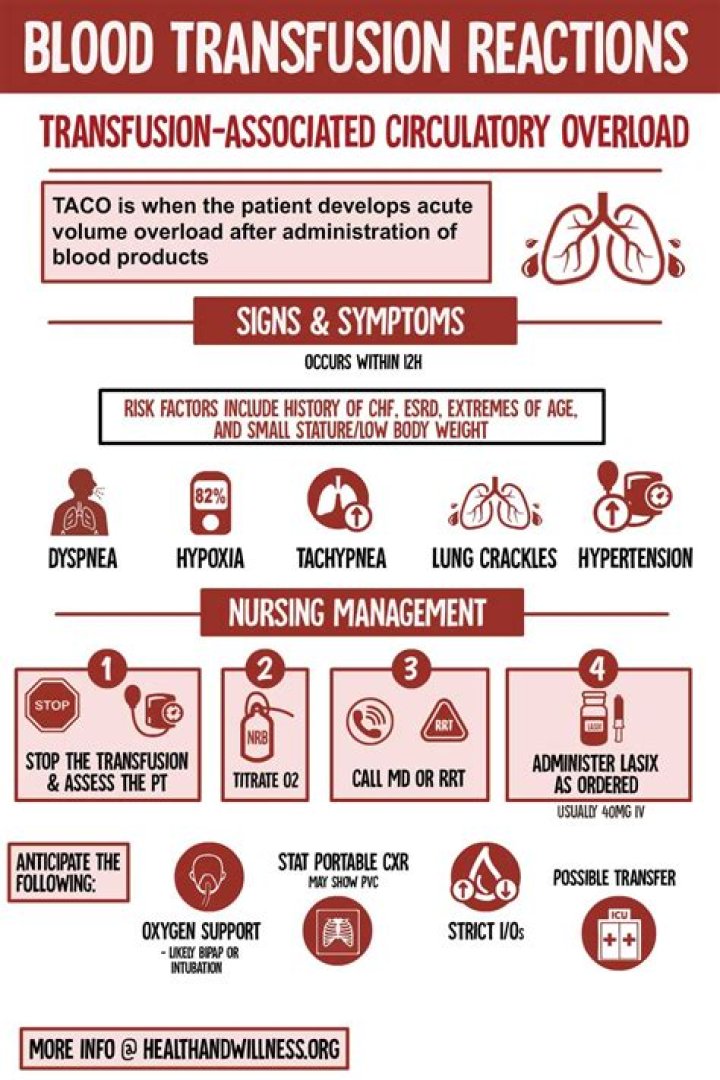
Transfusing 10 units of blood in a 24-hour period, or 5 units of blood in 4 hours, is considered a massive blood transfusion. Such a big blood transfusion replaces a large amount of the person's blood volume. A massive blood transfusion may be needed in cases where someone is in shock due to rapid blood loss.What are the signs and symptoms of circulatory overload?
Signs and symptoms include dyspnea, orthopnea, wheezing, tightness in the chest, cough, cyanosis, tachypnea, rapid increase in blood pressure, distended neck veins, and S3 on auscultation. Peripheral and pulmonary edema may also develop. Chest x-ray demonstrates bilateral infiltrates and possibly an enlarged heart.What are the different types of blood transfusion reactions?
Blood Transfusion Reactions- Acute Haemolytic Transfusion Reaction.
- Febrile Reactions.
- Allergic Reactions.
- Transfusion-Transmitted Infection.
- Transfusion-Related Acute Lung Injury.
- Transfusion-Associated Circulatory Overload.
- Delayed Haemolytic Transfusion Reactions.
- Transfusion-Associated Graft-Versus-Host Disease.
What is delayed hemolytic transfusion reaction?
DELAYED HEMOLYTIC TRANSFUSION REACTION. Delayed hemolytic transfusion reactions (DHTRs) present with red blood cell hemolysis from 2 days to several months after a transfusion. Symptoms and signs include fever, mild jaundice, and an inexplicable decline in hemoglobin concentration.Can a blood transfusion change you?
Although blood transfusions are much more frequent and have many connotations, derived from religious values, mass culture, or personal ideas, there is no study of the perception the patients have of changes in their behavior and values after a transfusion.What steps should be taken if a blood transfusion reaction occurs?
If you suspect a transfusion reaction, take these immediate actions:- Stop the transfusion.
- Keep the I.V. line open with normal saline solution.
- Notify the physician and blood bank.
- Intervene for signs and symptoms as appropriate.
- Monitor the patients vital signs.
What are risks of blood transfusion?
Allergic reactions, infections, fever, and iron overload risks and complications. Most blood transfusions go very smoothly. However, mild problems and, very rarely, serious problems can occur.What are the signs that you need a blood transfusion?
Possible risks and complications of blood transfusions| Reaction | Timing | Signs and Symptoms |
|---|---|---|
| "Delayed" hemolytic reaction | Within 3 to 7 days Up to weeks after the transfusion | Low-grade fever, mild jaundice (yellowing of the skin and whites of the eyes), decrease in hematocrit, chills, chest pain, back pain, nausea |