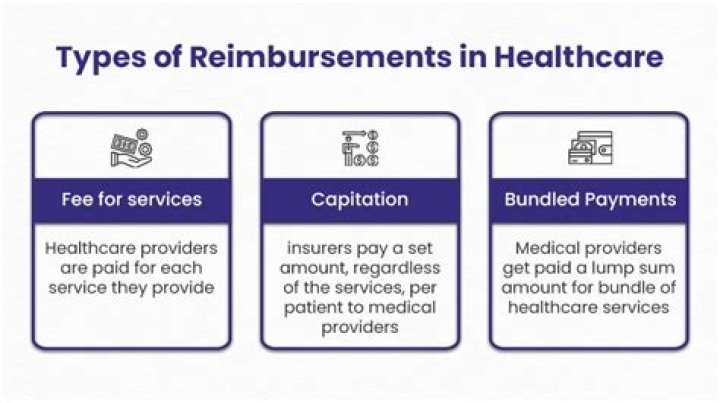
What are the major reimbursement methods used in health care?
.
Also know, what is the method of reimbursement?
The three primary fee-for-service methods of reimbursement are cost based, charge based, and prospective payment. Under cost-based reimbursement, the payer agrees to reimburse the provider for the costs incurred in providing services to the insured population.
Additionally, what is the most common form of reimbursement? The most common type of prospective reimbursement is a service benefit plan which is used primarily by managed care organizations.
Also asked, what are the different methods that MCOS reimburse providers for health care services?
Four payment methods (fee-for-service, discounted fee-for-service, capitation, and salary) and three payment adjustments (withholds, bonuses, and retrospective utilization targets) are the basis for nearly all contracts between health plans and your physicians, and they are described below.
How do reimbursements work in healthcare?
Healthcare reimbursement describes the payment that your hospital, doctor, diagnostic facility, or other healthcare providers receive for giving you a medical service. Typically, payment occurs after you receive a medical service, which is why it is called reimbursement.
Related Question AnswersWhat means reimbursement?
A reimbursement is a repayment for money you've already spent. When you travel for work, you get a reimbursement for your work-related expenses, like hotel bills and plane tickets, but you'll have to pay for that trip to the circus yourself. So the word reimbursement literally means in a purse again.What is a reimbursement model?
Under a bundled payment model, the payer reimburses all providers with a set price for the episode of care. This encourages the provider (in collaboration with the entire care team) to better manage the patients' care by avoiding preventable complications, like a hospital readmission.What is third party reimbursement?
Third party reimbursement is payment for services by an entity other than the patient or the patient's family. The provider and the patient are the two parties in the provision of health care services. A health plan becomes a third party when it is involved with reimbursing all or some of the service.What are the four basic modes for paying for healthcare?
The four basic modes of paying for health care are out-of-pocket payment, individual private insurance, employment-based group private insurance, and government financing (Table 2–1).What are cost reimbursement systems?
"Cost-based provider reimbursement" refers to a common payment method in health insurance. Under cost-based reimbursement, patients' insurance companies make payments to doctors and hospitals based on the costs of the care provided to the patients. Doctors speaking about paperwork with hospital accountant.What are the different types of payment systems in healthcare?
These methods are more specific than common terms, such as capitation, fee for service, global payment, and cost reimbursement. They also correspond to the division of financial risk between payer and provider, with each method reflecting a risk factor within the health care spending identity.What is a price based reimbursement methodology?
Price based reimbursement, is where the healthcare providers are paid a pre-set price for each service that they may provide. This price is determined by the services that the patients will receive.How does reimbursement affect patient centered care?
Quality of care is intrinsically tied to superior health outcomes and patient satisfaction. Value-based care reimbursement is pushing forward a more patient-centric healthcare delivery system, which can be clearly seen due to the creation of accountable care organizations and patient-centered medical homes.What is an example of fee for service?
Fee For Service. A method in which doctors and other health care providers are paid for each service performed. Examples of services include tests and office visits.What is an example of a managed care plan?
What are some examples of managed care plans? The most common type of managed care plan is the HMO. A third type of managed care plan is the POS, which is a hybrid of an HMO and a PPO. With a POS, you have to pick a primary care provider as with an HMO, but you also get to visit out-of-network providers as with a PPO.What are the different forms of payment to providers?
The three pure physician payment methods include: fee-for-service (FFS), capitation, and salary.What are the pros and cons of fee for service?
Pros: Flexibility. You can go to any medical provider, anywhere, without seeking plan approval first. Cons: Your total out-of-pocket costs will probably be higher than in a preferred provider plan or H.M.O. Most fee-for-service plans don't cover preventive care like flu shots or mental health services.What type of reimbursement does a PPO use?
A PPO is a healthcare benefit arrangement that is similar to an exclusive provider organization (EPO) in structure, administration, and operation. Unlike EPO members, however, PPO members are reimbursed for using medical care providers outside of their network of designated doctors and hospitals.What does professional courtesy mean?
Professional courtesy generally refers to the etiquette extended between members of the same profession. Some other well known groups that have some form of professional courtesy are attorneys, performing artists, and law enforcement officers.What are the advantages of fee for service?
Advantages. Patients receive highly valued service and the provider is able to offer suitable recommendations. Physicians can charge a reasonable amount for a plan and can be agile to offer precise assistance to their patients.What is the main difference between the fee for service and capitation reimbursement methods?
Capitation vs. Fee For Service. Capitation and fee-for-service (FFS) are different modes of payment for healthcare providers. In capitation, doctors are paid a set amount for each patient they see, while FFS pays doctors according to what procedures are used to treat a patient.What is a discounted fee for service?
Discounted Fee-For-Service. A financial reimbursement system whereby a provider agrees to supply services on an FFS basis, but with the fees discounted by a certain percentage from the physician's usual and customary charges. This may be a fixed amount per service, or a percentage discount.What are two reimbursement models?
The two models generally practiced around the US are fee-for-service (FFS) and value-based (VB) payment, which are in direct conflict.What are two types of payment models?
The key findings outline the six most common value-based payment models:- Medicare Quality Incentive Programs.
- Pay for Performance.
- Accountable Care Organization.
- Bundled Payments.
- Patient Centered Medical Home.
- Payment for Coordination.