Acute Myocardial Infarction in Patients With Diabetes Acute MI is a precipitating factor for DKA in approximately 4% of patients with diabetes who experience acute MI. During DKA events, the myocardium is denied glucose uptake because of high levels of ketones and free fatty acids, leading to myocardial ischemia..
Similarly one may ask, how does DKA develop?
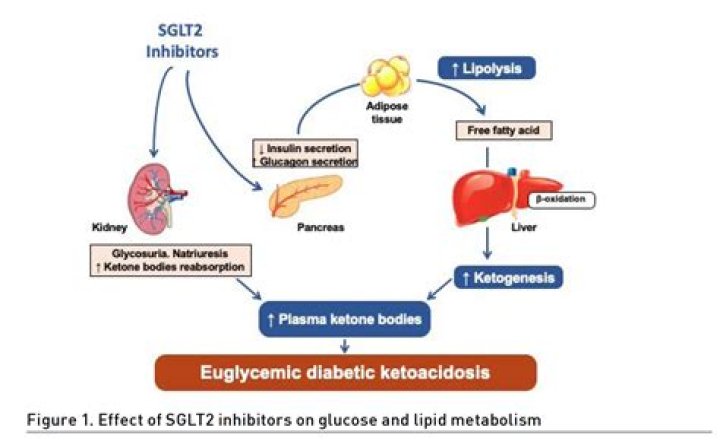
The condition develops when your body can't produce enough insulin. Without enough insulin, your body begins to break down fat as fuel. This process produces a buildup of acids in the bloodstream called ketones, eventually leading to diabetic ketoacidosis if untreated.
One may also ask, how does DKA affect potassium? Potassium levels can fluctuate severely during the treatment of DKA, because insulin decreases potassium levels in the blood by redistributing it into cells via increased sodium-potassium pump activity. A large part of the shifted extracellular potassium would have been lost in urine because of osmotic diuresis.
Likewise, can DKA cause elevated troponin?
In DKA, metabolic derangements, fluid shifts, tachycardia, and increased sympathetic tone may trigger focal myocardial necrosis and troponin I release due to cardiac ischemia from supply-demand mismatch, especially in patients with coronary artery disease (4).
How quickly does DKA develop?
SIGNS AND SYMPTOMS DKA can develop in less than 24 hours. 3 Metabolic changes occur one and one half to two hours earlier in patients who are managed only with a short-acting insulin such as lispro (Humalog).
Related Question Answers
Can you treat DKA at home?
If you detect ketones in your blood or urine, general treatment guidelines include drinking plenty of water or other calorie-free fluids to help flush ketones out of the body, taking insulin to bring your blood glucose level down, and rechecking both your blood glucose level and ketone level every three to four hours.What lab values indicate DKA?
While definitions vary, mild DKA can be categorized by a pH level of 7.25-7.3 and a serum bicarbonate level between 15-18 mEq/L; moderate DKA can be categorized by a pH between 7.0-7.24 and a serum bicarbonate level of 10 to less than 15 mEq/L; and severe DKA has a pH less than 7.0 and bicarbonate less than 10 mEq/L.What are the warning signs of diabetic ketoacidosis?
What are the symptoms of diabetic ketoacidosis? - frequent urination.
- extreme thirst.
- high blood sugar levels.
- high levels of ketones in the urine.
- nausea or vomiting.
- abdominal pain.
- confusion.
- fruity-smelling breath.
How do you test for DKA?
The ketone test is usually done using a urine sample or a blood sample. Ketone testing is usually done when DKA is suspected: Most often, urine testing is done first. If the urine is positive for ketones, most often beta-hydroxybutyrate is measured in the blood.What are the signs and symptoms of insulin shock?
Are There Symptoms of Hypoglycemia or Warning Signs of Insulin Shock? - Dizziness.
- Irritability.
- Moodiness or sudden changes in behavior.
- Hunger.
- Shakiness.
- Sweating.
- Rapid heart beat.
When should you go to the hospital for ketones?
A urine test for ketones should always be negative. Report a positive result to your doctor immediately. You should also let your doctor know right away if your blood sugar remains high or if you have stomach pain, nausea, vomiting, rapid breathing, sweet-smelling breath, or if you're urinating a lot.How often should you check ketones?
Many experts advise to check your urine for ketones when your blood glucose is more than 240 mg/dl. When you are ill (when you have a cold or the flu, for example), check for ketones every 4 to 6 hours. And check every 4 to 6 hours when your blood sugar is more than 240 mg/dl.Why is DKA so dangerous?
Diabetic ketoacidosis (DKA) is a dangerous complication of diabetes caused by a lack of insulin in the body. Diabetic ketoacidosis occurs when the body is unable to use blood sugar (glucose) because there isn't enough insulin. Instead, it breaks down fat as an alternative source of fuel.When should potassium be given in DKA?
Key DKA management points Start intravenous fluids before insulin therapy. Potassium level should be >3.3 mEq/L before the initiation of insulin therapy (supplement potassium intravenously if needed).What do you give for DKA?
Insulin Therapy Only short-acting insulin is used for correction of hyperglycemia. Subcutaneous absorption of insulin is reduced in DKA because of dehydration; therefore, using intravenous routes is preferable. SC use of the fast-acting insulin analog (lispro) has been tried in pediatric DKA (0.15 U/kg q2h).Why do you get hyperkalemia in DKA?
One example of potassium shift causing hyperkalemia is diabetic ketoacidosis. The acidosis and high glucose levels in the blood work together to cause fluid and potassium to move out of the cells into the blood circulation.What causes low potassium in DKA?
Potassium loss is caused by a shift of potassium from the intracellular to the extracellular space in an exchange with hydrogen ions that accumulate extracellularly in acidosis. Much of the shifted extracellular potassium is lost in urine because of osmotic diuresis.Is potassium low or high in DKA?
Total body potassium deficiency of 3-6 mEq/kg is expected at presentation of DKA due to osmotic diuresis, emesis, and secondary hyperaldosteronism; however, pretreatment serum potassium levels are usually not low due to the extracellular shift of potassium that occurs with acidosis and insulin deficiency (3, 4).What IV fluids do you give for DKA?
FLUID REPLACEMENT The initial priority in the treatment of diabetic ketoacidosis is the restoration of extra-cellular fluid volume through the intravenous administration of a normal saline (0.9 percent sodium chloride) solution.Why do DKA patients have abdominal pain?
Many mechanisms have been suggested to underlie the abdominal symptoms in DKA, namely acute hyperglycemia mediated impaired gastrointestinal motility (esophageal, gastric and gallbladder), rapid expansion of the hepatic capsule, and mesenteric ischemia precipitated by volume depletion.Is DKA considered critical care?
Patients with diabetic ketoacidosis (DKA) commonly are admitted to the intensive care unit (ICU). Patients automatically were deemed "appropriate" ICU admissions if they were older than 65 or had grade III or IV DKA, coma, co-existing conditions that required ICU care, shock, or hypothermia.How does insulin affect potassium levels?
The effect on potassium is clinically important. Insulin activates sodium-potassium ATPases in many cells, causing a flux of potassium into cells. Under certain circumstances, injection of insulin can kill patients because of its ability to acutely suppress plasma potassium concentrations.What does a diabetic attack feel like?
Anyone who experiences tiredness, increased thirst, frequent urination, or weight loss should see a doctor, as these could indicate diabetes or another health problem. A routine health check often involves blood sugar testing, even if the person has no symptoms.What is Kussmaul breathing?
Kussmaul breathing is a deep and labored breathing pattern often associated with severe metabolic acidosis, particularly diabetic ketoacidosis (DKA) but also kidney failure. It is this latter type of breathing pattern that is referred to as Kussmaul breathing.