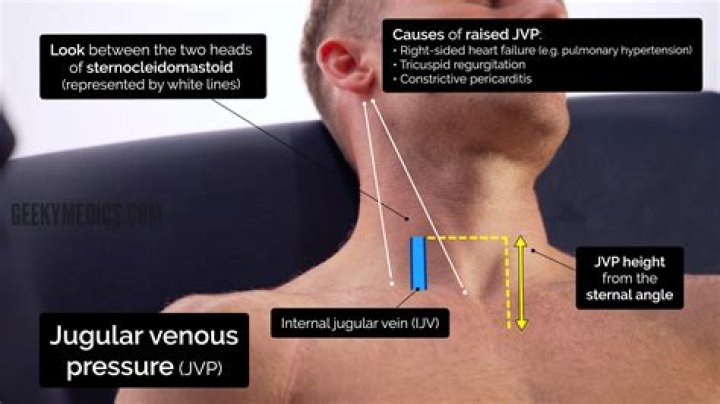
II. Technique: Jugular Venous Pressure measurement - Examine position. Head of bed elevated at 45 degree angle.
- Identify top of venous pulsation in neck (JVP) Jugular Venous Pulsations are inward.
- Identify the sternal angle (Angle of Louis)
- Measure distance between top of pulsation and Sternum.
.
Then, how do you check for jugular vein distention?
To help determine your CVP, your doctor will actually measure the height of the bulge. While you're lying down on an exam table, with the head of the table at a 45-degree angle and your head turned to the side, your doctor will measure the highest point at which pulsations can be detected in your internal jugular vein.
Also Know, how is JVP waveform measured? Techniques: Jugular Venous Pressure Measurement (JVP) Neck should not be sharply flexed. Using a centimeter ruler, measure the vertical distance between the angle of Louis (manubrio sternal joint) and the highest level of jugular vein pulsation. A straight edge intersecting the ruler at a right angle may be helpful.
One may also ask, what is the cause of JVD?
Jugular vein distention or JVD is when the increased pressure of the superior vena cava causes the jugular vein to bulge, making it most visible on the right side of a person's neck. However, there are other reasons why JVD might occur, such as a blockage.
What is normal JVP measurement?
Normal: JVP is 6 to 8 cm above the right atrium.
Related Question Answers
What does jugular vein distention look like?
Share on Pinterest Jugular vein distention is when a vein on the side of the neck appears to bulge. The appearance of the vein is similar to a rope or raised tube below the surface of the skin, and its height can be measured to indicate the CVP. An increased volume of blood and high CVP are signs of heart failure.Is jugular vein distention painful?
Circulatory symptoms that may occur along with jugular vein distention. Jugular vein distention may accompany other symptoms affecting the circulatory system including: Chest pain or pressure. Coldness of the fingers.Is it normal to see jugular vein pulsation?
non-palpable – the JVP cannot be palpated. If one feels a pulse in the neck, it is generally the common carotid artery. occludable – the JVP can be stopped by occluding the internal jugular vein by lightly pressing against the neck.What is Kussmaul sign?
Kussmaul sign is a paradoxical rise in jugular venous pressure (JVP) on inspiration, or a failure in the appropriate fall of the JVP with inspiration. It can be seen in some forms of heart disease and is usually indicative of limited right ventricular filling due to right heart dysfunction.Where is your jugular vein located?
They each rest beside the thyroid gland at the center of the neck, just above the collarbone and near the trachea, or windpipe. These veins functions to carry oxygen-depleted blood from the brain, face, and neck, and transport it to the heart through the superior vena cava.Why is my neck vein pulsating?
Abnormal pulses in a woman's neck were caused by a heart valve problem. This causes the right atrium to get bigger, and can change the pressure in nearby blood vessels, potentially leading to abnormal pulses seen in the neck veins, according to the American Heart Association.Why is my neck pulsing?
The carotid arteries take oxygenated blood from the heart to the brain. The pulse from the carotids may be felt on either side of thefront of the neck just below the angle of the jaw. This rhythmic beat is caused by varying volumes of blood being pushed out of the heart toward the extremities.What happens if the jugular vein is blocked?
"The jugular vein is an important body part because it drains deoxygenated blood from the head and the neck," Ashley tells Mental Floss. "Most important is to drain the brain. If you block the jugular veins, the pressure in the brain goes up."Is JVD a sign of dehydration?
Patients with suspected dehydration often have a history of vomiting, diarrhea, or decreased intake accompanied by volume-depleting medications (eg, diuretics). A physical examination of such a patient may demonstrate any or all of the following: Tachycardia. Absence of jugular venous distention (JVD).Why is JVP raised in heart failure?
Abstract. The internal jugular vein is observed to assess central venous pressure. The most common cause of raised JVP is congestive cardiac failure, in which the raised venous pressure reflects right ventricular failure (Epstein et al, 2003).Why do cardiologists look at your neck?
Your healthcare provider uses 2 fingers on each side of your neck to feel your carotid pulses. The right and left carotid arteries supply blood to your brain. Weak pulses could show a problem with the aortic valve or with the aorta. The aorta is the main blood vessel coming from the heart.How deep is the jugular vein?
The depth should be set to about 4 cm. The probe is moved medial to lateral to visualize first the carotid artery and then the jugular vein in cross section (Fig. 40-16).Can you see Pulse in neck?
You may feel your pulse in the arteries of your neck or throat. Sometimes you can even see the pulse as it moves the skin in a more forceful way. It may also feel like your heart is beating irregularly or that it has missed a beat, or like there is an occasional extra, more forceful heartbeat.What is right sided heart failure?
Right-sided heart failure means that the right side of the heart is not pumping blood to the lungs as well as normal. It is also called cor pulmonale or pulmonary heart disease.What does CVP mean?
central venous pressure
Which of the following is the best position for evaluating jugular venous distension?
To properly evaluate jugular venous distension, the patient must be placed at a 45 degree angle,or slightly less. Visualization of the jugular veins is best done at an oblique angle, so sit beside the patient and elevate the head of the cot into a semi-Fowler's position.How do you evaluate JVP?
3 It has been taught that the best method for evaluating the JVP is to position the patient supine in bed, elevate the patient's head to approximately 30–45 degrees, and measure or estimate the vertical height of the meniscus of the right internal or external jugular vein above the sternal angle (angle of Louis) whichIs JVP and CVP the same?
CVP estimates can be achieved by assessing the Jugular Venous Pressure (JVP), Peripheral Venous Collapse (PVC), and ultrasound visualization of the inferior vena cava (IVC). The CVP is considered elevated when the height of the internal or external JVP is >3 cm of vertical distance above the sternal angle [1]–[4].Why does JVP fall during inspiration?
JVP normally decreases during inspiration because the inspiratory fall in intrathoracic pressure creates a “sucking effect” on venous return. Thus, the Kussmaul sign is a true physiologic paradox. This can be explained by the inability of the right side of the heart to handle an increased venous return.