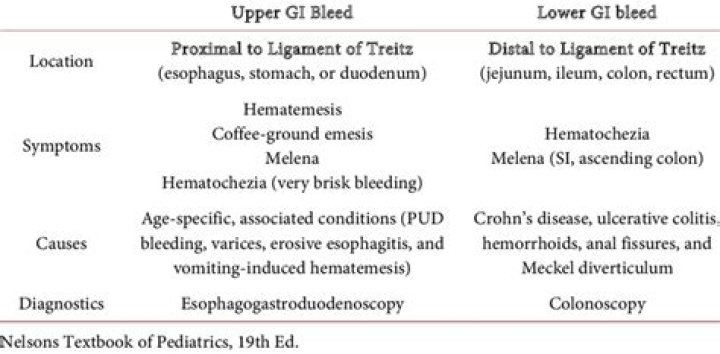
Historically, distinction of upper GIB (UGIB)and lower GIB (LGIB) was based on the location of bleeding in relation to the ligament of Treitz. With this definition, bleeding proximal to the ligament of Treitz is categorized as an UGIB, while bleeding distal to the ligament of Treitz is categorized as a LGIB..
Regarding this, how can you tell the difference between upper and lower GI bleeds?
Upper GI bleeding: The upper GI tract includes the esophagus (the tube from the mouth to the stomach), stomach, and first part of the small intestine. Lower GI bleeding: The lower GI tract includes much of the small intestine, large intestine or bowels, rectum, and anus.
Similarly, what is the most common cause of upper GI bleeding? Peptic ulcer. This is the most common cause of upper GI bleeding. Peptic ulcers are sores that develop on the lining of the stomach and upper portion of the small intestine. Stomach acid, either from bacteria or use of anti-inflammatory drugs, damages the lining, leading to formation of sores.
Moreover, how do you know if your GI tract is bleeding?
- black or tarry stool.
- bright red blood in vomit.
- cramps in the abdomen.
- dark or bright red blood mixed with stool.
- dizziness or faintness.
- feeling tired.
- paleness.
- shortness of breath.
What factors increase risk for GI bleed?
Some of the most common risk factors for nonvariceal UGIB include Helicobacter pylori infection, nonsteroidal antiinflammatory drugs (NSAIDs), aspirin, selective serotonin reuptake inhibitors, and other antiplatelet and anticoagulant medications.
Related Question Answers
What are the home remedies for GI bleeding?
There is no home care for heavy gastrointestinal bleeding. Hemorrhoids or anal fissures may be treated with a diet high in fiber, fluids to keep stools soft may be helpful, and stool softeners if necessary. Serious gastrointestinal bleeding can destabilize the vital signs of a patient.How do you rule out a GI bleed?
Upper endoscopy and colonoscopy are the mainstay of initial investigations. Angiography and radionuclide imaging are best suited for acute overt gastrointestinal (GI) bleeding. Capsule endoscopy and deep enteroscopy play significant roles in the diagnosis of obscure GI bleeding, usually from the small bowel.What test is used to detect gastrointestinal bleeding?
An endoscopy procedure may help your doctor see if and where you have GI bleeding and the bleeding's cause. Doctors most often use upper GI endoscopy and colonoscopy to test for acute GI bleeding in the upper and lower GI tracts. Upper GI endoscopy.Can a GI bleed heal itself?
Most hemorrhages are minor and not dangerous, and will clot and heal on their own. Many can be treated medically, sometimes with drugs that constrict blood vessels to close off bleeding. But when blood loss is ongoing or too fast, the GI team may seek to close off the bleeding in a more expeditious fashion.Would internal bleeding show up in a blood test?
Blood tests may be performed to check for a low red blood cell count, or anemia. However, if the bleeding occurs rapidly, the initial hemoglobin reading or red blood cell count may be normal. The suspicion of internal bleeding will often require an imaging test to look for the bleeding source.What is gastrointestinal bleeding?
Gastrointestinal bleeding (GI bleed), also known as gastrointestinal hemorrhage, is all forms of bleeding in the gastrointestinal tract, from the mouth to the rectum. When there is significant blood loss over a short time, symptoms may include vomiting red blood, vomiting black blood, bloody stool, or black stool.Is a GI bleed an emergency?
GI bleeding is a common cause of emergency department visits. A patient can be hemodynamically stable with hemeoccult positive stool or hemodynamically unstable and at significant risk of mortality with large volume blood loss. Generally, GI bleeding is categorized into upper and lower GI bleeds.What does a GI bleed smell like?
Black stool: This is usually foul-smelling and is caused by upper intestinal bleeding (stomach or upper small intestine, ulcers, or tumors. This is caused by hemorrhoids, colon polyps, rectal fissures, massive gastrointestinal bleeding, or colon cancer.How long does it take to recover from a GI bleed?
Even in the presence of a low Hb level at discharge, an acceptable outcome is expected after endoscopic hemostasis for nonvariceal upper gastrointestinal bleeding. Recovery of the Hb level after discharge is complete within 45 days.What is the most common cause of lower GI bleeding?
Colonic Bleeding Causes Colonic diverticulosis continues to be the most common cause, accounting for about 30 % of lower GI bleeding cases requiring hospitalization. Internal hemorrhoids are the second-most common cause.What medication can cause gastrointestinal bleeding?
Drugs that can lead to gastrointestinal bleeding include non-steroidal anti-inflammatory drugs (NSAIDs) like diclofenac and ibuprofen, platelet inhibitors such as acetylsalicylic acid (ASS), clopidogrel and prasugrel, as well as anticoagulants like vitamin-K antagonists, heparin or direct oral anticoagulants (DOAKs).Why do I bleed when I poop?
Seeing blood in the toilet, on the outside of your stool, or with wiping after a bowel movement is common. Fortunately, most of the causes of such rectal bleeding are not life-threatening; common causes include hemorrhoids and anal fissures. (See "Approach to minimal bright red blood per rectum in adults".)What causes Stomachbleeding?
There are many possible causes of GI bleeding, including hemorrhoids, peptic ulcers, tears or inflammation in the esophagus, diverticulosis and diverticulitis, ulcerative colitis and Crohn's disease, colonic polyps, or cancer in the colon, stomach or esophagus.Why am I bleeding from my butt?
Bright red blood may be seen only on toilet paper or in the toilet bowl after a bowel movement – not mixed freely with the bowel motion. This type of bleeding is usually caused by haemorrhoids (piles) or anal fissure. Both can be caused by constipation, and may cause difficult and painful bowel movements.Can you die from gastrointestinal bleeding?
Some patients who have a gastrointestinal bleed or perforation will die. Use of NSAIDs (non-steroidal anti-inflammatory drugs) or aspirin is likely to contribute to gastrointestinal bleeding and death.Can you feel colon cancer?
Signs and symptoms of colon cancer include: A persistent change in your bowel habits, including diarrhea or constipation or a change in the consistency of your stool. A feeling that your bowel doesn't empty completely. Weakness or fatigue.What does black tarry stool look like?
Black tarry stools Red blood cells are broken down by digestive enzymes in the intestine and turn the stool black. These stools tend to be tar-like (sticky) and foul smelling. This can be a medical emergency; black tarry stools should not be ignored.Can stress cause a GI bleed?
Stress-induced gastritis, also referred to as stress-related erosive syndrome, stress ulcer syndrome, and stress-related mucosal disease, can cause mucosal erosions and superficial hemorrhages in patients who are critically ill or in those who are under extreme physiologic stress, resulting in minimal-to-severeWhat does UGIB stand for?
Upper gastrointestinal bleeding (UGIB) is a common medical condition that results in substantial morbidity, mortality, and medical care cost. It commonly presents with hematemesis (vomiting of blood or coffee ground-like material) and/or melena (black, tarry stools).