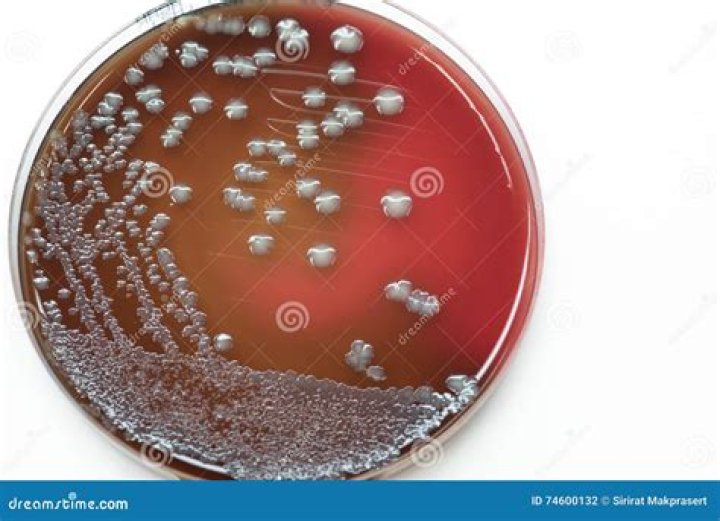
Isolation and Identification MacConkey and blood agar are usually used to isolate gram-negative bacteria, which usually grow within 24 to 48 hours and are subsequently differentiated on the basis of colony morphology and biochemical reactions. Pasteurella spp..
Also question is, what Bacteria grows on blood agar?
Blood Agar is used to grow a wide range of pathogens particularly those that are more difficult to grow such as Haemophilus influenzae, Streptococcus pneumoniae and Neisseria species. It is also required to detect and differentiate haemolytic bacteria, especially Streptococcus species.
Secondly, where are Gram negative bacteria found? The Gram-negative bacteria include most of the bacteria normally found in the gastrointestinal tract that can be responsible for disease as well as gonococci (venereal disease) and meningococci (bacterial meningitis). The organisms responsible for cholera and bubonic plague are Gram-negative.
People also ask, what is the morphology of gram negative bacteria?
They are characterized by their cell envelopes, which are composed of a thin peptidoglycan cell wall sandwiched between an inner cytoplasmic cell membrane and a bacterial outer membrane. Gram-negative bacteria are found everywhere, in virtually all environments on Earth that support life.
Can E coli grow on blood agar?
E coli is a gram-negative bacillus that grows well on commonly used media. It is lactose-fermenting and beta-hemolytic on blood agar. Most E coli strains are nonpigmented. Escherichia coli on Gram stain.
Related Question Answers
Does Salmonella grow on blood agar?
Bismuth sulfite agar: Salmonellae produce black colonies. Deoxycholate Citrate Agar (DCA): Salmonella appear as pale colonies. Eosin Methylene Blue (EMB) Agar: Non lactose fermenters, including Salmonella, Shigella and Proteus forms colorless or transparent colonies.Do all bacteria grow on blood agar?
No, the only thing that grows on blood agar is the bacteria because it breaks down RBCs. Blood agar is a differential medium because all the bacteria will grow on it due to the nutrients and iron. Patient A has streptococcus pyogenes due to the identical inoculation results from the blood agar plate.Why is blood agar differential?
Blood agar is a differential medium that distinguishes bacterial species by their ability to break down the red blood cells included in the media. Blood agar is often used to distinguish between the different species of pathogenic Streptococcus bacteria.Why is human blood not used in blood agar?
pneumoniae and S. pyogenes (1, 2, 3, 5). Agar prepared with human blood is not recommended, partly because of the safety risk to laboratory personnel, but mainly because it is said to result in poor bacterial isolation rates, although there are few published data to support this (2).What grows MacConkey Agar?
MacConkey Agar (MAC) is a selective and differential medium designed to isolate and differentiate enterics based on their ability to ferment lactose. Bile salts and crystal violet inhibit the growth of Gram positive organisms. Klebsiella pneumoniae ferments lactose and produces pink colonies on MAC.What does blood agar plate test for?
Blood Agar Plates (BAP) BAP tests the ability of an organism to produce hemolysins, enzymes that damage/lyse red blood cells (erythrocytes). The degree of hemolysis by these hemolysins is helpful in differentiating members of the genera Staphylococcus, Streptococcus and Enterococcus.What bacteria can grow on chocolate agar?
Chocolate agar is used for growing fastidious respiratory bacteria, such as Haemophilus influenzae and Neisseria meningitidis.What is blood agar selective for?
Blood agar media is used for the isolation and differentiation of Gram positive cocci, specifically Streptococcus species. So, it is selective for streptococcus. Blood agar is mainly used clinically to detect the presence of Streptococcus pyogenes, the human pathogen which causes "strep throat".What kills gram negative?
The outer membrane of Gram-negative bacteria plays an important role that is related to resistance to many antibiotics that are highly effective against Gram-positive bacteria, e.g. macrolides, novobiocin, rifamycin, lincomycin, clindamycin and fusidic acid.Why are Gram negative bacteria harmful?
As a rule of thumb (which has exceptions), Gram-negative bacteria are more dangerous as disease organisms, because their outer membrane is often hidden by a capsule or slime layer which hides the antigens of the cell and so acts as "camouflage" - the human body recognises a foreign body by its antigens; if they areWhat is a gram negative infection?
Gram-negative bacteria cause infections including pneumonia, bloodstream infections, wound or surgical site infections, and meningitis in healthcare settings. Gram-negative infections include those caused by Klebsiella, Acinetobacter, Pseudomonas aeruginosa, and E. coli., as well as many other less common bacteria.Is Gram positive or negative more dangerous?
In comparison to Gram positive, Gram-negative bacteria are more dangerous as disease organisms, due to the presence of capsule or slime layer which covers the outer membrane. Adopting this way, the micro organism can hide its surface antigens which required for triggering the human immune response.Does E coli have a thick cell wall?
In Gram-negative bacteria, the cell wall is only 1–3 layers thick (11), and in E. coli 80% or more of the peptidoglycan exists as a monolayer (12). Although the E. coli cell wall normally maintains a cylindrical shape during exponential growth (15), the cell shape can be altered either genetically or environmentally.Why are Gram negative bacteria pathogenic?
What Types of Bacteria Are Pathogenic? With this test, it was determined that Gram-negative bacteria are more resistant to antibodies because of their impenetrable cell walls. 90-95% of Gram-negative bacteria are pathogenic. On the other hand, many Gram-positive bacteria are non-pathogenic.Do gram negative bacteria have a cell wall?
In the Gram-negative Bacteria the cell wall is composed of a single layer of peptidoglycan surrounded by a membranous structure called the outer membrane. The gram-negative bacteria do not retain crystal violet but are able to retain a counterstain, commonly safranin, which is added after the crystal violet.Why is it more difficult to treat gram negative bacteria?
It is difficult to treat gram-negative bacteria in comparison to gram-positive bacteria due to following reasons. There is a membrane present around the cell wall of gram-negative bacteria which increases the risk of toxicity to the host but this membrane is absent in gram-positive bacteria.Why is E coli gram negative?
E. coli stains Gram-negative because its cell wall is composed of a thin peptidoglycan layer and an outer membrane.Is MRSA a gram negative bacteria?
MRSA, which most everyone knows about now, is gram-positive. We know about MRSA, but there has been an increase in infections caused by gram-negative bacteria, and they are resistant to many, or sometimes all, drugs.How long treat gram negative bacteremia?
Duration of Antibiotic Therapy for Uncomplicated Gram-Negative Bacteremia: Seven Is the New Fourteen. The treatment duration for uncomplicated gram-negative bloodstream infections (BSIs) has traditionally ranged from 7 to 14 days.